Bioindividual interpretation of a blood test in early pregnancy: The results aren’t what you expect
You may wonder why a blog about a blood test in early pregnancy even needs to exist…won’t the results and interpretation be the same as when a female isn’t pregnant? Or when she’s in her second or third trimester?
The short answer is: no.
The long answer, specific to the first trimester, is explained in this blog. And it will drastically change the way you interpret blood tests, how you treat pregnant patients, and, best of all, it will improve patient outcomes.
A blood test in early pregnancy produces surprising results due to major physiological changes
Yes, there are the obvious changes that occur during pregnancy. But females experience much more than a baby bump.
Maternal endocrine, immune, metabolic, and vasculature adjustments occur for and by the developing placenta and fetus.
For instance, the female’s anterior pituitary enlarges by two to three times its preconception size, while the thyroid gland increases by 18%.
Leptin levels double from preconception into the first trimester and continue to increase into the second and third trimesters. Leptin’s metabolic counterpart, ghrelin, begins its ascent in the first few weeks of pregnancy and gently peaks at mid-gestation, around 20 weeks (1).
Insulin and insulin-like growth factor binding protein 1 both increase in the first trimester (2, 3), as well.
While these changes are physiologically interesting, they are also clinically impactful. Blood test results in the different trimesters of pregnancy must be interpreted differently for the most accurate analysis.
A blood test in early pregnancy:
A bioindividual interpretation
Don’t worry: With this knowledge, you can understand why a blood test in early pregnancy needs special interpretation. Below are the specific markers to be aware of when working with pregnant patients.
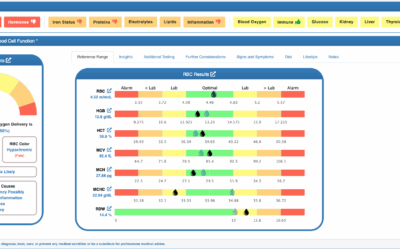
Red Blood Cells, Hemoglobin, and Hematocrit
One of the most impactful blood chemistry changes in pregnancy is a completely normal form of anemia called “dilutional anemia” or “physiological anemia of pregnancy.”
Because of hormonal changes that increase blood plasma volume, a female’s red blood cell count becomes diluted and, without proper range adjustment, reads as anemic during pregnancy.
Hemoglobin, the oxygen-carrying protein in red blood cells, and hematocrit, the percent of red blood cells in plasma by volume, also decrease beginning in the first trimester of pregnancy.
To learn more about this phenomenon, check out our blog on dilutional anemia in pregnancy.
First-trimester takeaway: RBCs, HGB, and HCT will be decreased and should be accounted for in the first trimester and throughout pregnancy.
Fibrinogen and D-dimer
Fibrinogen and d-dimer are interconnected blood markers that relate to our blood’s clotting ability. Fibrinogen is a protein made in the liver that helps blood clots to form, while d-dimer is a degradation product from the breakdown, or fibrinolysis, of blood clots.
Another normal change that begins in the first trimester of pregnancy is called physiological hypercoagulability. This is a necessary adaptation to protect pregnant females against bleeding during delivery, and generally, there are no clinical implications.
The hypercoagulability seen in pregnancy means that fibrinogen and d-dimer levels will be significantly higher in pregnant females versus non-pregnant females beginning in the first trimester.
However, be aware that nicotine use during preconception or pregnancy and gestational diabetes may lead to even higher levels of these markers. So if you’re working with a pregnant female with these influences, you may see higher levels of fibrinogen and d-dimer than in other pregnant patients (4, 5).
First-trimester takeaway: Fibrinogen and d-dimer will be elevated beginning in the first trimester and throughout pregnancy. Nicotinism and gestational diabetes may exacerbate this increase.
Alkaline Phosphatase
Alkaline phosphatase (ALP) is an enzyme that is primarily made and released into the blood from the liver and bones. During pregnancy, the placenta also creates and releases some forms of ALP into the maternal serum. However, higher production of maternal bone ALP also contributes to the two to three-fold increase seen in pregnancy (6).
ALP levels begin to rise during the first trimester and can remain elevated for up to six weeks after birth.
While a rise in ALP is normal during pregnancy, very high elevations can be a red flag for underlying problems. Gestational diabetes, hypertension, bone, hepatic, renal, or endocrine disease, or even heavy smoking may be related to extremely high levels of ALP during pregnancy (7, 8).
One crucial pattern of blood markers to be aware of in the first trimester is:
- Increased alkaline phosphatase
- Increased uric acid
- Increased gamma-glutamyl transpeptidase (GGT)
Research on over 1,000 pregnant females found that an increase in these three markers in early pregnancy may indicate an increased risk of gestational hypertension and pre-eclampsia (9).
First-trimester takeaway: Alkaline phosphatase will be elevated in early pregnancy with an up to 3-fold increase as pregnancy progresses. However, be aware of extremely elevated levels along with increases in uric acid and gamma-glutamyl transpeptidase.
TSH, free T4, and free T3
Thyroid-stimulating hormone, or TSH, is interesting because large but normal variations exist between individuals, while moderate normal variations exist within an individual.
This is one reason why the conventional range for TSH is so wide, sometimes as large as 0.5-5.0 mIU/L.
Ultimately, the best way to track thyroid function is to monitor intraindividual changes over time, i.e., compare the person to the person versus the person to the broad “normal” range. This step alone will lead to a more bioindividualized view of your patient’s TSH and thyroid function, especially when combined with the other thyroid hormones that will ideally accompany TSH, such as T4, T3, fT4, fT3, and perhaps reverse T3, T3 uptake, and appropriate thyroid antibodies based on symptom presentation (10).
But what about a thyroid blood test in early pregnancy? This gets tricky based on the wide variation.
However, TSH generally decreases in pregnancy due to the influence of placental human chorionic gonadotropin (hCG) and the increased synthesis of thyroxine-binding globulin related to elevated estrogen.
Free T4 and free T3, on the other hand, tend to increase in the first trimester and then gradually decrease in the second and third trimesters, though they stay within conventional reference ranges (11).
Beyond these changes, keep in mind that the endocrine and immune shifts that occur during pregnancy often trigger thyroid pathology in predisposed patients. So, due diligence for those with a strong family history or thyroid-related symptoms is a must.
First-trimester takeaway: TSH will decrease while TBG increases throughout pregnancy. Free T3 and free T4 will generally increase in the first trimester and then decrease as pregnancy progresses.
Automate your interpretation of a blood test in early pregnancy
If you’re looking for a way to speed up your research-backed interpretation of early pregnancy results, we’ve got your back. LabSmarts accounts for multiple blood test outcomes affected by pregnancy—you can keep seeing patients (and spending time with your family) while our software does the work.
Give your patients the results that only bioindividual book work interpretation can offer.
Learn more about how pregnancy impacts blood tests.
Sign up for our 6-week live masterclass…
“What You Never Learned About Blood Work in Preconception, Pregnancy, and & Postpartum.”
References
- https://www.ncbi.nlm.nih.gov/books/NBK278962
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4290225
- https://www.ncbi.nlm.nih.gov/gene/3484
- https://www.hindawi.com/journals/bmri/2020/3192350
- https://pubmed.ncbi.nlm.nih.gov/19935037
- https://pubmed.ncbi.nlm.nih.gov/3665032
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1770530
- https://www.degruyter.com/document/doi/10.1515/jpm-2020-0205/html?lang=en
- https://www.frontiersin.org/articles/10.3389/fcvm.2021.756140/full
- https://pubmed.ncbi.nlm.nih.gov/3708820
- https://academic.oup.com/bmb/article/97/1/137/359571