Is Iron Supplementation Safe?
Accurate analysis of anemia leads to fantastic client outcomes. But in the case of iron deficiency anemia, accurate analysis keeps your client safe.
In order to properly identify the possible root cause of your client’s anemia, levels of serum iron, ferritin, total iron binding capacity (TIBC), and iron saturation MUST be tested, along with of the red blood cell related markers on the complete blood count (CBC).
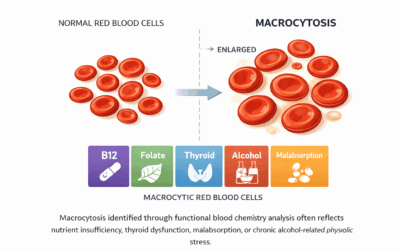
It’s important to understand that microcytic hypochromic anemia—when red blood cells are smaller and lighter red than what is optimal—is not always the result of iron deficiency. Recommending an iron supplement based solely on the values from the CBC alone can be harmful to your client. The study below illustrates how iron supplementation was deleterious to the mother and fetus based solely on the assumption that pregnant women should supplement with iron (1).

Without the results of all four iron-related markers, there’s still the question of whether to use supplemental iron or not. Why is this person’s hemoglobin low? Will supplemental iron resolve the issue, or make it worse? Ultimately, is iron supplementation safe?
Yes, but with some caveats.
Under the right circumstances, iron supplementation is not only safe but necessary and life changing! As clinicians, our job is to make sure that the right circumstances exist.
Your ability to properly identify patterns using all four iron-related markers will help you differentiate between a true iron deficiency anemia, when iron stores are low, or an instance of the body purposely keeping iron out of the serum (the liquid portion of blood).
In both cases, serum iron will be low. There are many possible causes of low serum iron, including a vegetarian or vegan diet, insufficient stomach acid, complications with nutrient absorption in the small intestine, and, the focus of this blog: bacterial infection.
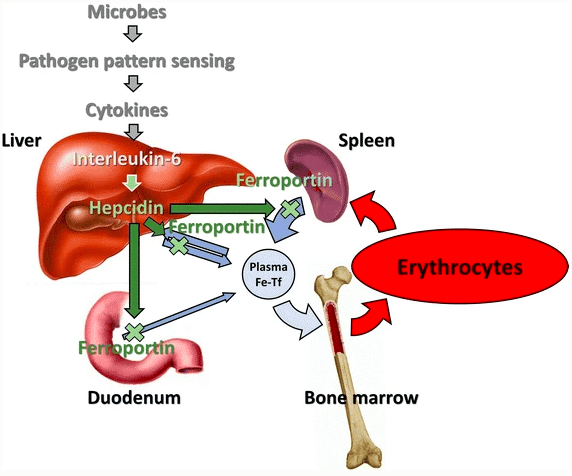
The body purposefully keeps iron out of the serum during bacterial infections.
Iron is like chocolate to bacteria.
Iron plays a big role in the evolution of many lifeforms, and bacteria are no exception. Microbes evolved ways to access iron in areas where not much was present, easily assimilate it, and even extract it from hosts…human hosts. This is called “iron piracy.” Thankfully, our innate immune system responds to iron piracy with “iron-targeted nutritional immunity,” multiple defense mechanisms that limit the amount of iron available to invading bacteria (2).
The interplay between bacteria, their hosts, and iron is exquisitely complex. While bacteria need iron to replicate, most bacteria also evolved to sense iron depletion (that occurs via nutritional immunity mentioned above) and thus recognize vertebrate hosts! Essentially, our bodies’ response to bacteria’s love for iron triggers microbes to know they’ve found a human home (3).
Obviously, iron supplementation is contraindicated during times of bacterial infection, even if iron deficiency anemia is apparent on a blood test. In fact, serum iron will normally decrease during infection or inflammation as part of immune defense mechanisms. The body knows to limit the amount of iron available to opportunistic bacteria (4).
When is iron supplementation safe?
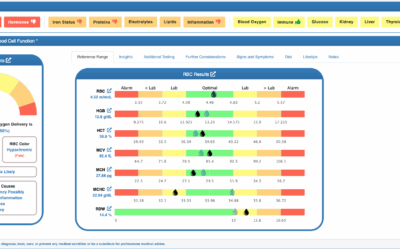
- The blood chemistry pattern of low serum iron, low ferritin, high TIBC, and low iron saturation is present.
- The blood chemistry pattern of low RBC, low HGB, and low HCT may also be present.
- White blood cells (WBC), neutrophils, lymphocytes, and the neutrophil to lymphocyte ratio (NLR) are within the optimal range for the individual.
When is iron supplementation not safe?
Indicators of bacterial infection include:
- Elevated WBCs and neutrophils typically indicate an acute bacterial infection.
- Decreased WBCs and elevated neutrophils typically indicate a chronic bacterial infection.
- Elevated Bands, which are young non-segmented neutrophils, indicate an active bacterial infection, even if WBCs are not elevated.
- Elevated NLR is indicative of a bacterial infection (5).
- Very high levels of CRP can indicate a bacterial infection but the studies are not definitive (6-10).
LabSmarts Can Help
LabSmarts’ pattern recognition engine identifies when an acute or chronic infection is a possible root cause of anemia, allowing you to make effective and safe iron supplementation recommendations (or not!).
References
- Lachili B, Hininger I, Faure H, et al. Increased lipid peroxidation in pregnant women after iron and vitamin C supplementation. Biol Trace Elem Res. 2001;83(2):103-110. https://pubmed.ncbi.nlm.nih.gov/11762527
- Ganz T. Iron and infection. Int J Hematol. 2018;107(1):7-15. https://pubmed.ncbi.nlm.nih.gov/29147843
- Skaar EP. The battle for iron between bacterial pathogens and their vertebrate hosts. PLoS Pathog. 2010;6(8):e1000949. https://pubmed.ncbi.nlm.nih.gov/20711357
- Zughaier SM, Cornelis P, eds. The Role of Iron in Bacterial Pathogenesis. Frontiers Media SA; 2018. https://www.frontiersin.org/research-topics/4986/role-of-iron-in-bacterial-pathogenesis
- Holub M, Beran O, Kaspříková N, Chalupa P. Neutrophil to lymphocyte count ratio as a biomarker of bacterial infections. Cent. Eur. J. Med. 2012; 7(2): 258–61. https://doi.org/10.2478/s11536-012-0002-3
- Tejani NR, Chonmaitree T, Rassin DK, Howie VM, Owen MJ, Goldman AS. Use of C-reactive protein in differentiation between acute bacterial and viral otitis media. Pediatrics. 1995;95(5):664-669. https://pubmed.ncbi.nlm.nih.gov/7724300
- Peltola H, Jaakkola M. C-reactive protein in early detection of bacteremic versus viral infections in immunocompetent and compromised children. J Pediatr. 1988;113(4):641-646. https://pubmed.ncbi.nlm.nih.gov/3262735
- Haran JP, Beaudoin FL, Suner S, Lu S. C-reactive protein as predictor of bacterial infection among patients with an influenza-like illness. Am J Emerg Med. 2013;31(1):137-144. https://pubmed.ncbi.nlm.nih.gov/22944552
- Escadafal C, Incardona S, Fernandez-Carballo BL, Dittrich S. The good and the bad: using C reactive protein to distinguish bacterial from non-bacterial infection among febrile patients in low-resource settings. BMJ Glob Health. 2020;5(5):e002396. https://pubmed.ncbi.nlm.nih.gov/32467355
- Durán A, González A, Delgado L, Mosquera J, Valero N. Serum level of C-reactive protein is not a parameter to determine the difference between viral and atypical bacterial infections. J Med Virol. https://pubmed.ncbi.nlm.nih.gov/26241406